IRANDERMA |
|
Quiz: September 2006 |
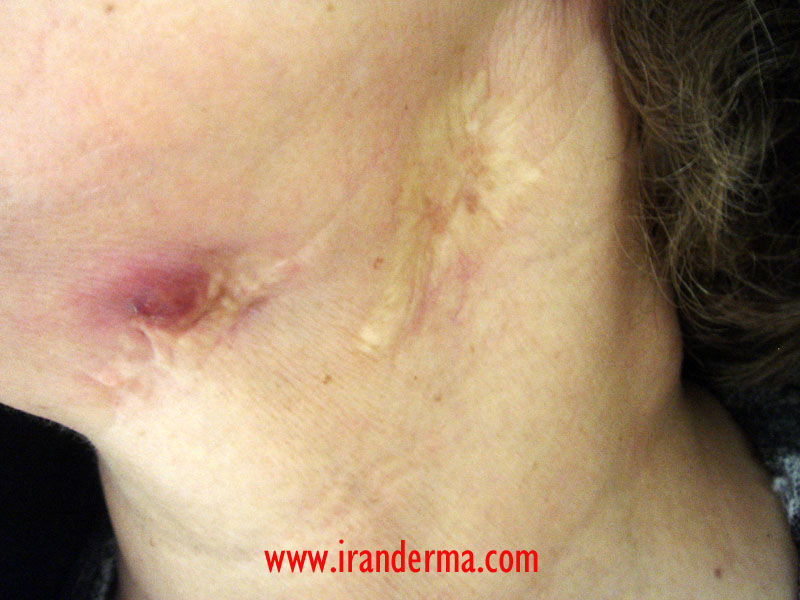
A 68-year-old woman referred for a long time history for a discharging nodule on her neck. Physical examinations revealed an old scar adjacent to the nodule and a large cervical lymph node at the same site. Otherwise she was healthy.
What is your diagnosis ?
Diagnosis: Scrofuloderma
Scrofuloderma
Synonyms: Tuberculosis Cutis Colliquativa, Tuberculoid Gumma
Scrofuloderma is a comprehensive term applied to tuberculous
involvement of the skin by direct extension, usually secondary
to underlying tuberculous lymphadenitis. It occurs most
frequently over the cervical lymph nodes, but may occur over
bone or about joints in children and young adults. Clinically
the lesions are reddish granulations, edematous, exudative, and
crusted, with small sinuses or ulceration of various size.
Generally cutaneous tuberculosis is an inflammatory process
caused by Mycobacterium tuberculosis. In the skin,
it may be primary as a consequence of direct inoculation
(tuberculosis verrucosa cutis) or secondary to a focus of
tuberculosis in another organ (the lung for lupus vulgaris, and
bones, as well as lymph nodes, for scrofuloderma). In the
elderly, with decreased immunity, there may be hemogenous spread
with seeding of subcutaneous fat.
The
process for scrofuloderma ususally begins with deep purpulish
induration of the skin overlying diseased lymphatic glands,
which for months have been matted together and doughy. The glans
tend to break down and the resulting purulent and caseous
exudate stretches the superimposed skin and forms fistulas in
it. Chronic discharging sinuses and oval or linear ulcerations,
irregular pale granulations, bulky crusts, hypertrophic scars,
and cicatricial bands result, and these combined conditions
composed scrofuloderma.
Laboratory Finding
Cutaneous tuberculosis includes all forms of tuberculosis affecting the skin—those in which organisms can be identified (tuberculous ulcer, scrofuloderma, orificial tuberculosis, tuberculosis verrucosa cutis, and lupus vulgaris) as well as those conditions formerly called "tuberculids" (erythema induratum, papulonecrotic tuberculid, lichen scrofulosum). In all cases, tissue biopsies for culture should be performed. Often in the later conditions, cultures and polymerase chain reaction studies fail to detect mycobacteria, but antituberculous treatment is still indicated.
Diagnostic indicated tests are :
- Tuberculin skin test (tine test; Mantoux) induces a papule at the site of injection in a person who has developed delayed hypersensitivity to M. tuberculosis.
- Acid-fast organisms can be demonstrated in smears from ulcers.
- Culture of tissue from biopsy specimens of skin may verify the diagnosis.
- Polymerase chain reaction is effective in demonstrating mycobacterial DNA in tissue sections of skin biopsy specimens.
Differential Diagnosis
- Scrofuloderma is to be differentiated from syphilitic gummas, which when ulcerated, form deep craters;
- Sporotrichosis, which yields the typical fungus when cutured;
- Blastomycosis, as demostrated by presence of Blastomyces dermatitidis,
- Lymphogranuloma venereum is rule out by a negative LGV complement fixation test,
- Scrofuloderma should also be differentiated from actinomycosis and tularemia by culture.
Treatment
- All patients with cutaneous tuberculosis should receive multidrug therapy.
- Duration of therapy should be at least 6 months.
- Single drug treatments and shorter courses are NOT recommended.
- A standard regimen might include isoniazid (INH) 300 mg, rifampin (RIF) 600 mg, pyrazinamide 20–30mg/kg, and ethambutol 15–20 mg/kg daily for 2 months, then INH and RIF daily for 4 months more.
Comment:
Mehrdad
Mehravaran, M.D., Dermatologist
Szeged-Hungary
ايران درما |